Learn more about...
Scoliosis
Curvature of the Spine
Scoliosis is a three-dimensional curvature of the spine that can develop in childhood or adolescence, causing the vertebrae to twist and bend to the side. While mild curves often go unnoticed, more severe curves can lead to uneven shoulders, hips, or ribcages, and may impair lung and heart function if left untreated. Early detection and monitoring are key, since growth spurts can accelerate curve progression. Though there’s no “cure” for the change in alignment, modern therapies aim to halt progression and, in many cases, partially reverse the curve.
Diagnosis
Screening
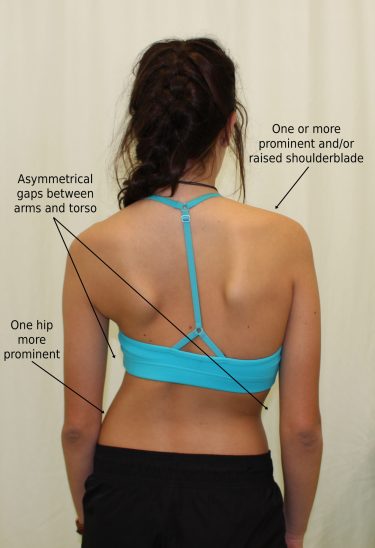
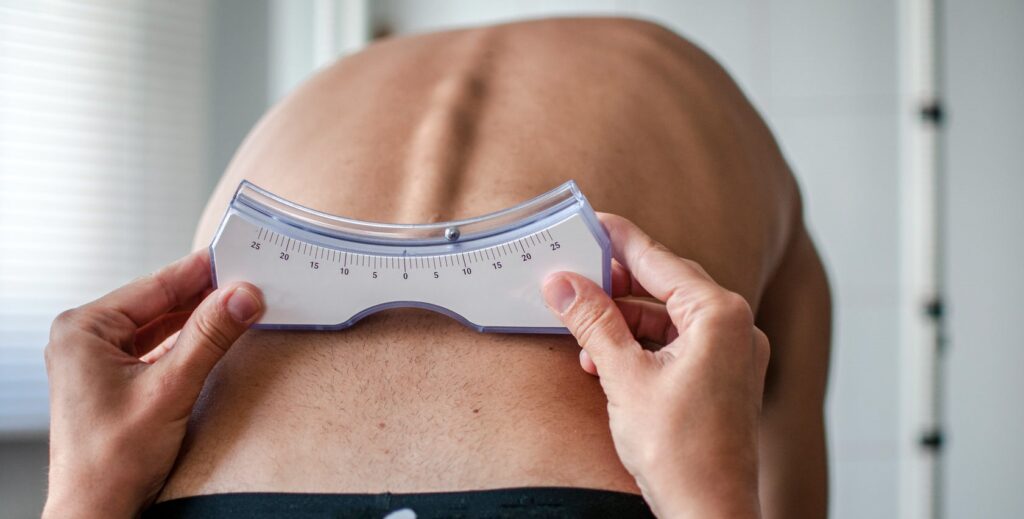
Screening for scoliosis typically begins with a simple physical exam—your provider will look for asymmetries in the shoulders, waist, and hips and may ask you to bend forward to check for rib prominence (the Adam’s forward-bend test). If a curve is suspected, standing X-rays of the full spine are taken to measure the Cobb angle, which quantifies the degree of curvature. For children and teens, follow-up imaging is scheduled every few months during growth to watch for changes. In some cases, MRI may be ordered to rule out underlying spinal cord or nerve issues.
Cause
Nerve Tension
At its core, scoliosis often reflects an adaptive posture: as the vertebral bones grow faster than the spinal cord can stretch, tension builds along the cord’s length. To relieve that nerve tension, the body instinctively shifts the spine into a curved position, distributing stress more evenly. This compensatory mechanism helps protect the spinal cord from overstretching but, over time, produces the characteristic “S”- or “C”-shaped alignment. While growth-related imbalance is the most common trigger, genetics and neuromuscular conditions can also play a role.
Treatment
1) Curve Reduction Phase
Over the first 18–24 months, intensive therapies—posture drills, strength training, specialized equipment, and bracing—work together to actively straighten the spine. Four- to five-day inpatient intensives occur every three months, maximizing Cobb-angle improvements during rapid growth. This phase is critical: most of the measurable curve correction happens here, especially early on.
2) Stabilization Phase
Once maximum reduction is reached (typically after two years), the goal shifts to holding that correction. Bracing continues 23 hours per day while chair-based therapies taper off, and shorter, two- to three-day intensives every three months reinforce progress. This phase prevents the curve from rebounding until growth plates begin to close.
3) Weaning Phase
After 24–36 months and skeletal maturity (Risser 4–5), brace hours are gradually reduced—usually by four hours every three to four months—until only night-time wear remains. This slow transition supports muscle strengthening and helps the spine “lock in” its new alignment.
4) Observation
In the final, skeletally mature stage, care moves to one-day follow-ups every six to twelve months. These visits include baseline exams and imaging to confirm long-term stability. At this point, most patients discontinue brace use entirely, though periodic check-ins continue into adulthood to ensure lasting results.